We understood that failing to maintain normothermia can cause numerous complications and realized the inconsistency of our facility’s temperature measurement practices created the possibility of hypothermia going undetected in a significant
number of patients.
Staff at different points of the perioperative process would use various temperature reading methods: oral, rectal, temporal artery, esophageal and pulmonary artery. In fact, we identified instances of inconsistent temperature taking throughout
the surgical encounter for the same patient. Each of these methods had varying reliability, which created inconsistency in our ability to determine which patients were hypothermic and how big of an issue we faced in ensuring staff applied
active warming methods appropriately and properly.
The core temperature is the most accurate temperature source with less variation caused by environmental factors. In the past, the use of invasive devices was the only option for capturing core body temperature readings, a factor that limited
their use and availability for relatively minor surgical procedures. Our goal was to implement a consistent, reliable and easy-to-use non-invasive method of recording temperatures in all phases of surgical care. We decided to implement a standardized
monitoring system after trialing a non-invasive core temperature measurement device that hospital stakeholders approved for purchase. The device utilizes a single-use sensor that sticks to the patient’s forehead and quickly delivers
an accurate temperature reading. It can be used through each phase of care, allowing for clinical efficiency and accuracy.
Nursing and anesthesia staff members from all perioperative settings received training on using the temperature-taking device. Implementation of the standardized program was successful after providers completed the learning curve, troubleshooting
took place and validation of the initial data collection was obtained. Initial findings showed unintended hypothermia was a much more significant issue than we previously thought; informal data gathering suggested 45% of our patients were
hypothermic.
Staff were unsure whether to trust the volume of hypothermic patients initially detected with the new device, as it recorded temperatures that were much lower than values recorded with traditional temporal artery probes. The literature reports
that temporal artery values are an acceptable reflection of core temperature in the normothermic patient, but unreliable for temperatures outside the normothermic range.
Staff appreciate the ease with which they can transfer data from the non-invasive devices into our hospital’s electronic medical record. The collection of accurate and standardized temperature readings provides an easier way to conduct audits
that focus on how compliance with temperature-taking protocols and active warming practices impacts rates of hypothermia among surgical patients.
Our initial investigation into the higher-than-expected rates of surgical complications and the collection of accurate temperatures along the perioperative pathway alerted us that our patient warming protocols needed to be standardized. Every
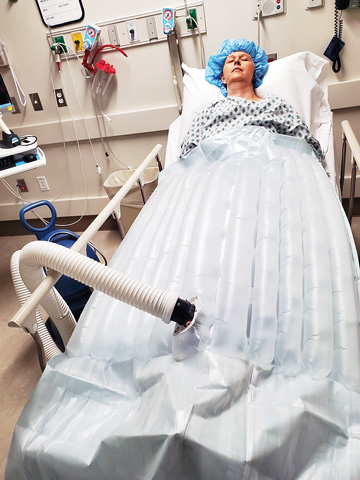
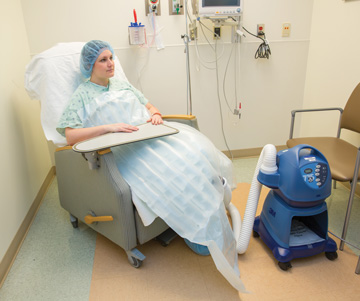
patient in pre-op is now given a forced-air warming gown; they feel more involved in their care by being able to control the temperature of the gown and adjust it to their level of comfort.
The constant flow of warm air circulating through the gown elevates peripheral body temperature, not core body temperature. This active pre-warming technique reduces the temperature gradient from core to peripheral areas. When patients arrive
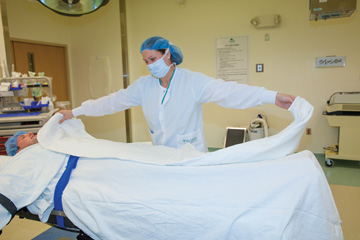
in the OR, a forced-air warming blanket and other modalities are used to maintain their core body temperatures and reduce heat loss. Postoperatively, warming gowns are reapplied and utilized until patients meet criteria for discharge from
the recovery unit.
.svg?sfvrsn=be606e78_3)
.svg?sfvrsn=56b2f850_5)