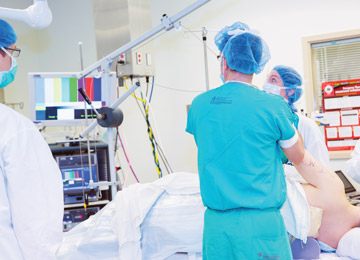
Patients are placed laterally or in the beach chair position for most shoulder procedures. “Both require surgeons to have access to the front and back of the joint as they’re maneuvering scopes and instruments,” says Rothman’s Dr. Horneff.
To gain the 360-degree access needed during arthroscopies, surgeons place multiple portal sites posteriorly, anteriorly and laterally.
“The posterior portal is the main access point,” says Edward Westerheide, MD, of Orthopedic Specialists & Sports Medicine in Newark, Ohio.
Dr. Horneff says seeing and working in and around the shoulder capsule can prove challenging. “We have specialized cameras with a bit of angulation, which helps visualization,” he explains, “but we’re also [manipulating instruments] through an anterior portal. That’s why it’s important to have unimpeded access at the front of the joint.”
That can be tricky, depending on how the patient is positioned, says Dr. Westerheide. “As you’re maneuvering instruments, they can butt up against the patient’s head,” he explains. To prevent this, Dr. Westerheide places the head in a forward-leaning position, making sure the cervical spine isn’t flexed forward.
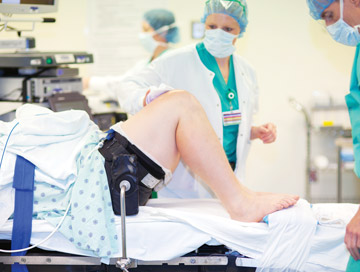
There are a number of different shoulder tables available that give your surgeons extra precision and access. “Most of the good tables have a hydraulic-assist component,” says Dr. Westerheide. “Instead of having to manually lift up the table while keeping the patient’s head stable, a spring-elevated lever does a lot of the work for you.”
The shoulder table Dr. Westerheide uses also has a hydraulic positioning component that locks the patient’s arm in whatever position he chooses. “You step on a pedal and place the arm where you want it, then simply step off the pedal to lock the arm in place,” he explains. That easy maneuverability lets him easily set forward flex and abduction of the joint.
Dr. Horneff says that during open procedures, such as shoulder replacements, surgeons establish access with an anterior incision and must be able to move the patient’s arm freely in space without worrying about the surgical table impeding the motion.
The most challenging aspects of performing a shoulder replacement involves accessing and viewing the glenoid, according to Dr. Horneff. Pneumatic or mechanical arm holders let him position the arm in various positions to help him achieve both goals. “To access the glenoid, you bring the patient’s arm up in an external rotation with abduction to help the humerus fall [away from the field],” comments Dr. Horneff. “Arm positioning aids make that so much easier to do.” OSM
.svg?sfvrsn=be606e78_3)
.svg?sfvrsn=56b2f850_5)